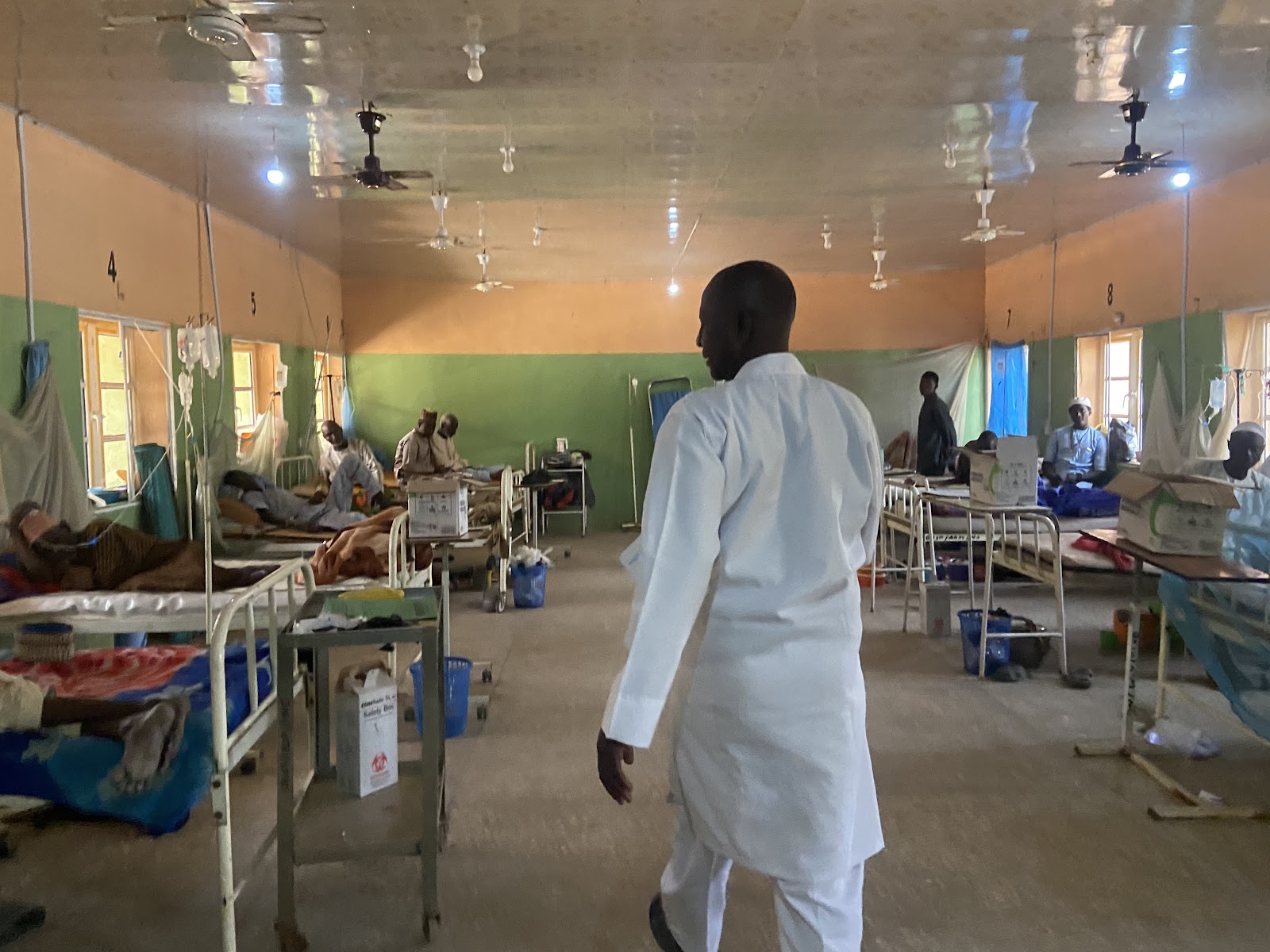
BY ABUJAH RACHEAL
When the Federal Government appropriated N218 billion for health capital projects in 2025, hospitals across Nigeria anticipated long-overdue renovations, diagnostic equipment upgrades, and infrastructure expansion.
However, what the hospitals received instead was N36 million, representing just 0.0165 per cent utilisation, the lowest capital release performance in Nigeria’s health sector in at least a decade.
For frontline workers at General Hospital, Calabar, Cross River, the consequences are both immediate and visible
The facility, recently upgraded with a redesigned reception, consulting rooms, a pharmacy, and an emergency theatre, is meant to serve as a vital bridge between primary and tertiary care.
Yet, modern infrastructure has not translated into improved service delivery.
“Sometimes we have to ask patients to buy syringes, gloves, or even basic medication before we can treat them,” a nurse who requested anonymity told the News Agency of Nigeria (NAN).
In spite of being earmarked for major improvements under the 2025 health capital allocation, the hospital received only a fraction of the expected funds.
Essential equipment remains unused, procurement processes have stalled, and members of staff improvise daily. Across Nigeria, similar stories are unfolding.
Capital Without Cash – Allocation vs Actual Release 2016–2025
An analysis of federal budget data from 2016 to 2025 shows that in 2016, 53 per cent of the N28.7 billion appropriated for health capital was released.
In 2017, the release improved to 65 per cent, while in 2018 and 2019, implementation hovered between 55 and 60 per cent.
In 2020, during the COVID-19 pandemic, utilisation stood at 50 per cent; in 2021, implementation peaked at 70 per cent, with N93.8 billion released from N134 billion appropriated.
Nonetheless, the decline began in 2022, when utilisation dropped to 45 per cent.
In 2023, it fell further to 30 per cent, and in 2024, only 15.06 per cent of the original N434.8 billion allocation was released.
By 2025, the system effectively worsened, delivering less than 0.02 per cent of the intended funds.
Experts describe the shift from 70 per cent implementation in 2021 to 0.0165 per cent in 2025 as more than fiscal strain; they say it is a structural breakdown.
Dr Emmanuel Sokpo, Country Director of the Network for Health Equity and Development, raised deeper concerns about transparency.
Sokpo questioned how capital financing sourced from loans, grants, and development partners was reflected in official budget execution records.
“There is what appears to be a black pot in health financing; the total inflow and outflow of funds are never fully clear,’’ he said.
He said that without consolidated disclosure of loan-backed infrastructure projects, counterpart funding, and external grants.
Sokpo said it became nearly impossible to assess the true volume of resources entering the health sector.
Observers say the lack of clarity raises difficult questions: Is the low release due to cash-flow constraints? Is debt servicing crowding out capital spending? Are funds being reallocated through virement? Or are administrative bottlenecks stalling disbursement?
As of press time, no detailed public breakdown explained the 2025 shortfall.
Dr Uzodinma Adirieje, Programmes Director of Afrihealth Optonet Association, described the situation as a national development emergency.
“When capital investments collapse, economic productivity declines, educational outcomes suffer, social grievances intensify, and fiscal inefficiencies expand,” he said.
Adirieje warned that chronic underinvestment erodes Nigeria’s demographic dividend and weakens national resilience.
Experts say the implications extend beyond infrastructure–Nigeria’s proposed 2026 health allocation of N2.9 trillion represents just 4.98 per cent of the N58.47 trillion national budget, far below the 15 per cent commitment under the 2001 Abuja Declaration.
Meanwhile, out-of-pocket expenditure remains among the highest in Africa, with citizens reportedly paying up to 95 per cent of health costs directly.
In Nasarawa State, Mrs Halima Audu delayed her child’s vaccination after her local Primary Health Centre ran out of vaccines due to procurement delays.
“I had to travel over 20 kilometres to another facility. Many mothers cannot afford that,” she said.
In Bendeghe Ekiem, Cross River, Nurse Anikan Mark said infrastructure expansion projects had halted.
“Patients waiting for maternal and child health services experience long delays. Some resort to informal providers,” Mark said.
Experts warn that such gaps increase risks of preventable deaths, treatment delays, and catastrophic household spending.
The Health Sector Reform Coalition Nigeria called for a legislative investigation into the 2025 capital release.
Its chairman, Dr Mohammed Lecky, described the near-total non-release as “one of the most alarming failures in recent health governance history.”
A health economist, Dr Abigail Banji, advocated for legally binding cash-backed budgeting, ring-fenced capital funds, milestone-based releases, and independent audits.
Predictable funding, Banji said it was critical not only for healthcare delivery but for national productivity and security.
While Nigeria struggles with execution, Rwanda and South Africa have demonstrated consistent fiscal discipline in meeting the Abuja benchmark.
Dr Emmanuel Agogo noted that allocating funds on paper was insufficient.
“Allocating money on paper is onething; spending it effectively is another,” he said.
Without disciplined implementation, infrastructure investments risk remaining symbolic.
From 70 per cent implementation in 2021 to 0.0165 per cent four years later, Nigeria’s health capital financing has entered uncharted territory.
Stakeholders warn that unless transparency improves, fiscal discipline strengthens, and cash-backed budgeting becomes mandatory, capital allocations may continue to exist only on paper.
And in hospitals like Calabar’s General Hospital, where equipment sits idle and patients are asked to supply basic materials, the cost of “capital without cash” is paid daily, in delayed care, financial hardship, and diminished trust in the system.
Release Percentage Trend (2016– 2025) – Visual decline from 70% to 0.0165%.
Dr Aminu Magashi, Coordinator of the African Health Budget Network (AHBN) and a health economist, proposed reforms to stabilise Nigeria’s health financing.
Magashi called for cash-backed budgeting and ring-fenced capital funds, including allocations for the Basic Healthcare Provision Fund, vaccine procurement, essential life-saving drugs and commodities, alongside performance-linked releases to ensure that funds were available and tied to project milestones.
He emphasised integrated fiscal governance and transparency measures, including clear disclosure of loans, grants, and counterpart funding, complemented by regular budget-tracking meetings.
He also recommended donor alignment, treating health allocations as first-line charges, and mobilising domestic revenue, such as allocating at least 50 per cent of sin-tax proceeds to healthcare.
Magashi argued that the aforementioned steps would establish a predictable, transparent, and resilient system capable of supporting infrastructure, service delivery, and broader national development.
By the foregoing, it has become imperative for the National Assembly, fiscal authorities, and health policymakers to urgently enforce cash-backed budgeting, guarantee transparent capital releases, and ring-fence funds for infrastructure, vaccines, and essential life-saving commodities.
Ultimately, health advocates warn that without immediate reform, Nigeria’s health budget will remain a promise on paper, and citizens will continue to pay the price in care delayed, costs transferred, and trust eroded.